How to Get a Better Night’s Sleep

Overview
Sleeping problems are one of the most common complaints reported by people experiencing stress and those who are seeking therapy. Common sleeping difficulties can include problems falling asleep, problems staying asleep, and oversleeping.
Unfortunately (and paradoxically), the activities that we typically engage in when we cannot sleep are often the very things that unintentionally stimulate us and keep us awake. Fortunately, the majority of sleep difficulties are easily remedied by examining our pre-sleep routine and our response to sleeping difficulties.
The information on this page first explains ‘why’ we need sleep, including what happens to our brains and bodies during each of the 4 Stages of Sleep. Following this, practical solutions are recommended to help you get a better night’s sleep.
Given the well-established link between sleep disturbance and our ability to handle stress, striving to achieve good quality sleep consistently is one of the most beneficial Self-Care investments that we can make to better manage and to improve our psychological well being.
Why do we Sleep?
Sleep is an important part of our daily routine: We spend about one-third of our lifetimes doing it. Good quality sleep (getting enough of it and at the right times) is as essential to survival as food and water. We now know that prolonged sleep deprivation leads to a poorer immune system, increased agitation and susceptibility to depression, anxiety, and psychotic symptoms, and can even increase our risk of developing cancer.
Sleep is a complex and dynamic process that affects how we function. From the latest science, we now know that sleep is important to a number of brain functions, including how nerve cells (neurons) communicate with each other. Recent findings suggest that sleep plays a housekeeping role (‘synaptic pruning’) that removes toxins in our brain that build up while we are awake.
Without adequate sleep, we cannot form or maintain the pathways in our brain that let us learn and create new memories (‘memory consolidation’). You may have noticed that with poor sleep, it is harder to concentrate, we have more negative thoughts, and we are more likely to become impatient and irritable. Basically, without good quality sleep, we cannot function at our psychological best.
Sleep also affects almost every type of tissue and system in the body – from the brain, heart, and lungs to metabolism, immune function, mood, and disease resistance. Research shows that a chronic lack of sleep, or poor quality sleep, not only increases the risk of psychological problems but also medical problems including high blood pressure, cardiovascular disease, diabetes, and obesity.
How Much Sleep Do We Need?
There is no “magic number of sleep hours” that works for everybody because our need for sleep changes across the lifespan. Babies sleep as much as 16 to 18 hours per day, which may boost growth and development (especially of the brain). School-age children and teens on average need about 9.5 hours of sleep per night. On the other hand, most adults need between 7-9 hours of sleep a night. For adults 60 years and older, sleep tends to be shorter, lighter, and increasingly interrupted by multiple awakenings.
Alarmingly, people of all ages are getting less sleep than they need due to longer work hours and the availability of round-the-clock entertainment and other activities. Most of us mistakenly assume that we can “catch up” on missed sleep. Yet, sleep deprivation studies show that we never actually make up for the total number of minutes lost. Moreover, sleep deprivation impacts on our psychological well-being. We know from resent research (here and here) that sleeping less than 4 hours a night for one week can trigger psychotic symptoms in healthy adults (!). So clearly, irrespective of your age, not getting the sleep that you need has harmful effects both in the short and long term.
What happens when we sleep?
Sleep Cycles
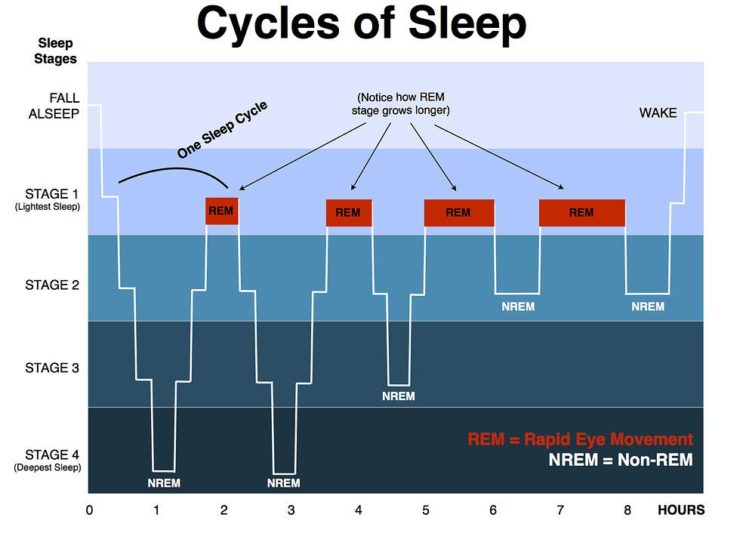
What is a Sleep Cycle? A sleep cycle is a complete progression through all of the sleep stages (see diagram below) from light to deep sleep, then reversing back from deep sleep to light sleep. This cycle ends with time in REM sleep, before starting over again.
How long is a sleep cycle? The first sleep cycle takes about 90 minutes. After that, each cycle lasts between 100 to 120 minutes. Typically, we go through four to five sleep cycles a night. Periods of wakefulness most often occur between the various sleep stages or when we shifts sleeping positions.
The Stages of Sleep
While sleep is often thought of as a passive process, research has shown that the brain is actually quite active during different stages of sleep. Sleep plays an important role in a number of processes, including learning and memory consolidation and neural pruning (i.e., a ‘brain clean-up’ process that improves the efficiency of our brain much like re-booting a computer does).
There are two basic types of sleep: Rapid eye movement (REM) and non-REM sleep. Non-REM sleep has different stages which include ‘Delta’ sleep – the deepest stage of sleep that leaves us feeling the most refreshed.
Each stage of sleep is linked to specific brain waves and neuronal activity. Normally, we cycle through all stages of non-REM and REM sleep several times during a typical night (this is called a ‘sleep cycle’), with increasingly longer, deeper REM periods occurring towards morning.
Sleep disturbances can occur for a variety of different reasons and can affect different stages of sleep, depending on the problem. For instance, we know that memory consolidation (an important part of ‘learning’) happens during REM sleep which is often affected in people with PTSD and trauma. Interestingly, there are therapies that facilitate the processing of ‘stuck’ trauma memories by having clients recount these memories while performing eye-movements similar to those observed in REM sleep.
Non-REM Sleep
Stage 1 – Muscle tone throughout the body relaxes and brain wave activity begins to slow from that of wake. Some people may experience sudden jerks or muscle spasms of the entire body (called hypnic jerks) or they may even experience sensation of falling while drifting in and out of Stage 1. Brain waves begin to slow from their daytime wakefulness patterns. This drowsy sleep stage can be easily disrupted causing awakenings or arousals.
Stage 2 – This is the period of light sleep before we enter deeper sleep. Our heartbeat and breathing slows, and our muscles relax even further. Our body temperature drops and our eye movements stop. Brain wave activity slows but is marked by brief bursts of electrical activity.
Stage 3 & 4 – The hallmark of this stage of sleep are the slowest brain waves (Theta & Delta waves). These waves are responsible for ‘deep sleep’ – Deep sleep provides the most restorative sleep of all the sleep stages. This is what we need in order to feel refreshed in the morning.
During deep sleep, muscles relax and the heartbeat and breathing slow to their lowest levels. Human growth hormone is released and restores the body and muscles from the stressors of the day. The body repairs and regrows tissues, builds bone and muscle, and strengthens its immune system.
Often it is difficult to awaken someone in deep sleep. Parasomnias (sleepwalking, sleep talking or somniloquy and night terrors) occur during the deepest stage of sleep. Unfortunately, as we age, we sleep more lightly and get less deep sleep. Melatonin and exercise (discussed below) can help us spend more time in Delta each sleep cycle.
Much less is known about deep sleep than REM sleep.
REM sleep
REM sleep is important and is worthy of a mention on its own. Most dreaming occurs during REM sleep and it is responsible for memory consolidation and learning. During REM sleep, our eyes move rapidly from left to right behind closed eyelids. As can be seen in the diagram above, REM sleep occurs at the end of each sleep cycle.
We know from research that disruptions in REM sleep (as caused by alcohol and other substances) can lead to difficulties with learning new material, concentration and problem solving during wakefulness. Interestingly, we also know that people who are disturbed by stress and / or unprocessed traumatic memories (such as those with high levels of anxiety, depression, or PTSD symptoms) have significant problems with their REM sleep.
A therapy for trauma called Eye Movement Desensitization & Reprocessing (EMDR) Therapy makes use of the left-to-right eye movements that occur in REM sleep to help people process traumatic and painful experiences, and following EMDR Therapy people’s sleep improves. EMDR Therapy is approved by the world health organization as a first-choice treatment for trauma. I have written about EMDR therapy here.

Dreaming
Everyone dreams. We spend about 2 hours each night dreaming but may not remember most of our dreams. Its exact purpose of dreaming is not known, but dreaming may help us process our emotions. For instance, we know that events from the day often influence our thoughts during sleep. We also know that people dream about the relationships in ways that characterize their attachment styles (I discuss this further in this article here), and we know that people suffering from stress or anxiety are more likely to have frightening dreams.
Dreams can be experienced in all stages of sleep but usually are most vivid in REM sleep. Some people dream in colour, while others only recall dreams in black and white. Parasomnias (sleepwalking, sleep talking or somniloquy and night terrors) occur during the deepest stage of sleep.
Poor Sleep & Mental Health: The Vicious Cycle
Poor sleep directly affects our mental health. Overwhelming amounts of studies consistently demonstrate that insufficient, or poor sleep leads to irritability, fatigue and low mood. A recent sleep restriction study found that restricting sleep to 4 hrs per night for just three consecutive nights, leads to psychotic symptoms in healthy adults (significant increases in paranoia, hallucinations, and cognitive disorganization). Relative to the control condition, participants in the 3-day sleep restriction condition reported significant increases in negative affect, negative ‘self-‘ and ‘other-‘ cognitions, increases in worry, and impairments in working memory. This is simply from having sleep restricted for three nights.
It probably comes as no surprise that poor sleep can have a negative impact on problem-solving and transfusion tolerance, and can exacerbate stress, anxiety, and depressive symptoms (simply Google: ‘Sleep + Mental Health‘). And we know that there is a reciprocal relationship: People with mental health difficulties experience poor sleep AND poor sleep leads to mental health difficulties! If you are experiencing these latter difficulties you should definitely seek help to work on the underlying issues.
If you are only willing to change one thing about the way that you sleep – do this: Set an alarm at the same time every day and stick to it no matter how late you go sleep the night before. This is the simplest (although not easiest) way to regulate our sleep-wake cycle.
‘Snoozing’ & Oversleeping
Do you reach for the alarm ‘snooze’ button? Most people think that ‘more sleep is better’ and that ‘not enough sleep’ is the only problem we can have with sleep. However, oversleeping can cause just as many problems as under-sleeping.
Firstly (and you have probably experienced yourself): Oversleeping can make us feel sluggish. Often this is because when we hit ‘snooze’ we are entering a brand new sleep cycle. However, when we wake-up next, we are effectively mid-way through the next sleep cycle. At other times, sluggishness from oversleeping can be due to us throwing off our biological clock which can trigger confusion in our minds and body that mimics ‘jet lag’.
In addition to mental fogginess, oversleeping has been associated with: Back pain, weight-gain, headaches, diabetes, heart disease, and depression.
Symptoms of oversleeping include:
-
-
- Sleeping for extended hours at night (typically well beyond the 7-8-hour general norm)
- Difficulty waking up in the morning (including sleeping through an alarm)
- Trouble rising from bed and starting the day
- Grogginess consistently throughout the day
- Trouble concentrating
-
Oversleeping & Depression – Sleep and depression have a complex relationship. Disrupted sleep is both a symptom of and a contributing factor to depression. Most people with depression experience regular sleep disturbances (they do not sleep well and do not feel ‘refreshed’ from sleep). This is problematic because we know that sleep problems can make depression more severe and more difficult to treat.
Oversleeping can be used as an ‘avoidance strategy’ (to avoid stress or challenging emotions). We know that ‘avoidance’ only works in the short term, but over time it often makes us feel worse about our situation and ourselves. Unsurprisingly, avoidance is a common response in many mental health difficulties (including depression and anxiety).
Oversleeping may also be related to having a disrupted sleep-wake cycle, such as in people who have become ‘nocturnal’ (again, also very common in depressive and anxiety disorders).
Hypersomnia – Oversleeping may also be a symptom of hypersomnia (a medical condition causes people to suffer from extreme sleepiness throughout the day, which is not usually relieved by napping). Many people with hypersomnia experience symptoms of anxiety, low energy, and memory problems as a result of their almost constant need for sleep. Similarly, oversleeping may be a symptoms of obstructive sleep apnoea, a disorder that causes people to stop breathing momentarily during sleep, can also lead to an increased need for sleep, because it disrupts the normal sleep cycle.
Although oversleeping is not necessarily indicative of an underlying mental health difficulty or a sleep disorder, if after following the guidelines on this page you still find it difficult to get your sleep-wake cycle in check it might be a good idea to consider visiting a Sleep Clinic that can monitor your brain’s activity while you are trying to sleep, in order to better determine what is going on.

How to Get a Better Night’s Sleep
If you want to improve your sleep quality and wake feeling ‘refreshed’, it is also important to examine what you are doing before you go to sleep. Below is a comprehensive list of things that you can do to take back the power and have a good night’s sleep.
As you read through this list, take note of which areas you know you need to address. If you are engaged in therapy, your therapist will likely have many creative ways to help you address these issues.
Technology Use: Melatonin & Dopamine
‘Screen time’ is the most common lifestyle reason for difficulties people have with falling asleep. Why? The blue-light frequencies that are emitted by all modern back-lit devices (TVs, Laptops, Tablets, Kindles, and Smartphones) disrupts our body’s production of Melatonin – a sleep-inducing hormone that normally gives us that ‘wave of sleep’ feeling to help us fall and stay asleep! We now know from studies of the brain that even when we include a ‘buffer’ of no screens before bedtime, people who use technology before sleep produce lower levels of melatonin compared to people who do not use technology.
This study compared caffeine vs blue-light and found BOTH had significant effects on alertness psychomotor and cognitive function. In other words, blue-light is as stimulating as caffeine. The researchers concluded that blue-light has “the potential to positively influence a range of settings where cognitive function and alertness are important”.
So, unless you want to increase your alertness before bedtime, the science tells us to turn off all screens at least 2 hours before bedtime and do something soothing and calming to wind-down (eg, meditate, go for a walk, have a bath or shower, read a book, do a puzzle, do some therapeutic writing). This gives your brain a chance to begin to produce Melatonin which helps us fall (and stay) asleep. Melatonin also helps us sleep deeper which means we wake feeling refreshed (vs ‘hung over’ from technology use).
Note. Another problem with using any entertainment device before bedtime is that the interaction with a device is a source of cognitive, tactile and visual stimulation that operates on ancient reward-circuitries in the brain (i.e., dopamine) and this stimulation runs counter to the calm states we require to fall asleep.
Use a Blue-Light Screen-Filter
If you must use technology before bedtime, download and install a Blue-Light Filter on all of your technology devices. These filters are typically synchronized to start as the sun sets. They cut down the blue-light produced by our screens by introducing a reddish-pink overlay.
An example of a Blue-Light Filter is f.flux (for PCs & OSX), Night Screen (for Android Devices). Some newer model iPhones have ‘Night Shift’ – a blue-light filter – built in. Use a Blue-light filter on every device you own. Its ‘set & forget’ so you never need to think about it. If you do not use a Blue-Light Filter, you will be interfering with your body’s production of the sleep-inducing hormone, Melatonin (see below).
However, this needs to be re-stated: Although screen filters can reduce your exposure to blue-light, they are an imperfect solution because they still allow some blue-light to pass through. In addition, the interaction with a device is a source of cognitive and visual stimulation that operates on ancient reward-circuitries in the brain (i.e., dopamine) and this is counter to the calm states required to fall asleep.
Again, if you want to act on the most current information we have to: limit your screen use before sleep by at least 2 hours. This sounds simple, but many people have used devices at night for such a long time that they need to (re-) discover what other activities are soothing and conducive to winding down.
Again, having a buffer of no screen time before bed, gives your brain a chance to begin to produce Melatonin which helps us fall (and stay) asleep. More Melatonin also means we will sleep deeper which means we wake feeling refreshed (vs ‘hung over’ from technology use).
Melatonin Tablets
Melatonin is a sleep-inducing hormone produced naturally in the brain by the pineal gland. It is a light-sensitive process that requires darkness to trigger it, so exposure to bright light (eg Blue-Light from technological devices, or very bright lights) before bedtime halts your body’s natural production of this valuable hormone.
Research confirms that melatonin decreases sleep onset latency (how long it takes to fall asleep) and it increases total sleep time and improves overall sleep quality (external links to three recent large scale studies here, here, and here). Melatonin is safe (non-toxic) is drug-free, and is non-addictive. However, as will be discussed, not all Melatonin supplements are created equally.
Please be aware – 5-10 mg Melatonin is the most common dose reported in many clinical trials. Yet, in Australia, we can only purchase 1-2mg Melatonin tablets and this requires a prescription (yes, we have Melatonin sold over the counter but this is deceptively labelled ‘homeopathic strength’, which is scientifically meaningless. What this really means is that over-the-counter Melatonin is much weaker than prescription strength Melatonin, which in Australia is still weaker than the 5-10mg dosage used in scientific studies worldwide).
An alternative option is to purchase Melatonin in 5mg strength tablets (the dosage reported in most clinical trials) online in either ‘regular’ or ‘slow-release’ tablets, depending on whether you have trouble falling or staying asleep, respectively.
Note. Melatonin is not a sleeping pill and its effects are very subtle (and are weakened by blue light, sugar and caffeine). For best results, take Melatonin on an empty stomach (about an hour after dinner) approximately 40 mins before bedtime.
Taking a Melatonin supplement will not over-ride the negative effects of blue-light from a screen. If you are serious about sleep, you still need to limit your screen time at night and implement a buffer of ‘no screens’ within 1.5-2 hours of bedtime. This is what your brain needs to recover from blue-light exposure and to begin to make more melatonin. This is not my opinion, it is science.
Exercise
We know from research that people who exercise regularly sleep deeper and subsequently feel more refreshed when they wake. The reason for this is that people who exercise actually spend more time in the ‘delta’ (deepest) stage of sleep – which is responsible for making you feel rejuvenated and energized from sleep. Because we have several sleep cycles every night, the more time you spend in ‘delta’, the more refreshed you will likely feel.
Exercise is a great way to kick start our metabolism in the morning but it may not fit in with your routine. Although some exercise is better than none, we know that strenuous exercise can actually stimulate our stress hormones and this can interfere with sleep – So, try to aim to complete any vigorous exercise at least 4 hours before bedtime to give your body time to calm down from the physiological stimulation.
Caffeine and Sugar:
Tea, coffee and chocolate all contain caffeine (a stimulant). Although there is research suggesting caffeine affects sleep even consumed 6 hours before bedtime, I recommend avoid drinking coffee after midday if you are serious about sleep. More about caffeine here. Refined sugar also has a stimulating effect and can keep you awake, so if you are having trouble sleeping it may be time to reassess your sugar intake and find an alternative.
Alcohol
We know from research that alcohol interferes with quality of REM sleep and that disruptions in REM sleep lead to difficulties with concentration and problem solving. Avoid drinking alcohol if you want a good night’s sleep.
Nicotine
Nicotine is a stimulant and makes it harder to fall asleep and to stay asleep. Avoid smoking (or gum / patches) at least 2 hours before bed.
Bed is for Sleeping
Animals learn about their environments through contextual cues – so do humans! If we use our bed as a place to surf the Internet, engaged in social media, watch TV, eat, read, work on your laptop, or any other thing that stimulates our mind, our brain learns this connection and we come to associate being in bed with being alert and entertained. Try not to use your bed for anything other than sleeping so that you come to associate your bed with just one thing: sleep.
Problem Solving
If you still can’t fall asleep after 20-30 mins then it may actually help to get up and do something that is calming and does not involve the use of a screen or any other kind of bright light (eg read a book in dim lighting in a chair away from your bed, or do a puzzle under dim lighting).
The idea behind this is to focus on something else until you start to feel drowsy and the wave of sleep returning – this will give you something else to do that is not too stimulating (vs becoming frustrated about just lying there, which can actually stimulate you unnecessarily). This strategy can also help if you wake in the middle of the night and are unable to fall asleep after some time. Get up and do something low-light and low in stimulation until the next wave of sleep returns.
Another useful activity is writing – This can also be useful after you have failed to fall asleep after trying for a period of 20-30 mins, or when we wake up in the middle of the night and find ourselves wide awake thinking….
What? Getting things out of our minds and on paper can often clear out the mental chatter that can keep us awake.
How? – Get up, grab a pen and a notepad and start writing. Write about things that may be on your mind, or engage in a therapeutic writing task, or write a list of things your mind would like to do but you currently cannot currently do because it is late at night. All of these things will now be out of your mind and committed to a piece of paper for you to address in the morning or at some later stage when the time is right.
Summary
- Sleep is important for many reasons, including learning and memory.
- Sleep disturbance is often related to stress. Stress can impact on our sleep quality and poor sleep can negatively affect our ability to handle stress.
- Poor sleep is both a symptom and a cause of mental health problems (and interestingly, psychosis has been triggered in healthy adults limited to 4hr per night of sleep which highlights just how important good quality sleep is).
- Sleep difficulties can include: Difficulties falling asleep, difficulties staying asleep, and oversleeping. Each problem requires a specific solution.
- In general, there are many things that you can do to help yourself get a better night’s sleep, with the simplest being: to stick to the same wake-time every morning, no matter what. Over time, this will correct most sleep issues.
- To help give yourself the best chance of falling asleep, there are a range of actions you can take in the hours leading up to sleep. The the most important of these are to: Use a blue-light filter on all devices with screens, and to switch off technology at least 2hrs before bedtime. These sleep hygiene behaviours allow our brain to produce and release Melatonin, which helps us fall (and stay) asleep.
- Although Melatonin supplements can help, they need to be of sufficient strength (5-10mg is the dosage reported in the latest research), taken on an empty stomach, and are not a substitute for switching off devices at least 2hrs before bedtime.
- Improving your sleep is an important aspect of Self-care that will help with your energy levels, your mood and frustration tolerance, and your ability to handle stress.
If you are continuing to have difficulties getting a good night’s sleep or if you would like assistance with managing ongoing difficulties and distress in your life, I recommend that you seek the professional assistance of an experienced Clinical Psychologist who can tailor their approach to your unique situation. After all, if you could have solved your sleep (and other) issues on your own, you probably already would have.
To learn how you can get the most out of therapy, I have prepared the following article.
Further Resources
- Learn about how to deal with negative thinking
- Calm your body & mind with Soothing Rhythm Breathing
- Learn about mindfulness
- Your brain’s 3 Emotion Regulation Systems
- Processing traumatic experiences with EMDR Therapy
- Watch a fascinating TED talk – by Circadian Neuroscientist Dr Russell Forster (external link: Why our brain’s need sleep )
- For all articles that I have written visit here