Understanding Obsessive Compulsive Disorder (OCD)
People with OCD experience-anxiety provoking thoughts that are intrusive, distressing and unwanted that they can’t get rid of (obsessions). In an attempt to manage obsessive thoughts, and reduce their anxiety about their thoughts, people often engage in repetitive rituals (compulsions) which they acknowledge are excessive and unreasonable. An example may be someone washing their hands repeatedly and excessively to manage fears of contamination or illness. However, often the ritualised behaviours can begin to take over people’s lives.
The reason why people persist in engaging in compulsions is because they have not learned to respond to their anxious thoughts in ways that are workable. Like all other anxiety disorders, people are simply being pushed around by their mind’s thoughts, and this activates their brain’s threat system. In addition, for people with OCD, they have also incorrectly ‘linked’ up in their minds that certain behaviours are functioning to keep them safe, because performing them causes a temporary relief in their anxious thoughts and feelings.
This is actually a seductive trap. It results in a self-reinforcing feedback-loop between the anxious obsession and the behavioural compulsion, because people mistakenly deduce through a process of ’emotional reasoning’ that the behaviours they are engaging in are actually doing something to keep them safe – because they ‘feel’ less anxious after performing the compulsion. This becomes a very powerful reinforcer, and the OCD continues.
What is needed is a combination of skills that draw upon Mindfulness, self-regulation, and reality-testing, combined with a thorough understanding of the brain’s emotion regulation systems. With such an understanding, these skills will facilitate engaging in Exposure therapy, which is an individually tailored way to perform reality-testing and to learn through experience that the compulsions do not actually serve their assumed function. This new learning can upgrade and replace old unquestioned habitual ways of responding to what your mind is doing and can set you free again.
Understanding Obsessions (vs Compulsions)
Obsessions are intrusive, unwanted thoughts, images, or urges usually about negative or catastrophic events or outcomes. Obsessions are typically accompanied by intense and uncomfortable feelings such as anxiety, fear, shame, disgust, doubt, or a feeling that things have to be done in a way that is ‘just right’, or something ‘bad’ might happen…
Compulsions are repetitive behaviors or mental acts performed to reduce the distress caused by obsessions or to prevent a feared outcome. In short, obsessions create anxiety, and compulsions are attempts to relieve it.
Common obsessions:
Contamination
- Environmental contaminants (e.g., chemicals, asbestos, radiation)
- Body fluids (examples: urine / faeces)
- Germs/disease, or Dirt
Obsessions Related to Perfectionism
- Concern about evenness / exactness
- Concern with a ‘need to know’ or remember
- Inability to decide whether to keep / discard things
- Fear of losing / forgetting important information when throwing something out
- Fear of losing things
- Obsessions about sexuality
- Forbidden / perverse sexual thoughts / images / impulses
- Religious Obsessions (Scrupulosity)
- Concern with offending God (blasphemy)
- Excessive concern with right/wrong or morality
Losing Control
- Fear of acting on an impulse (e.g., to harm oneself / others)
- Fear of violent or horrific images in one’s mind
- Fear of stealing things
- Fear of blurting out obscenities or insults
Harm
- Fear of being responsible for something terrible happening
- Fear of harming others because of not being careful enough
Moral Scrupulosity
- Obsessive concern about being immoral, unethical, or having committed a wrongdoing—even when there’s little or no evidence—often leading to excessive confessing, seeking reassurance, or avoiding situations where one might act “improperly.”
Other Obsessions
- Preoccupation with getting a specific disease (e.g. cancer)
- Superstitious ideas (e.g., lucky/unlucky numbers; certain colours)
Understanding Compulsions
Compulsions are performed to relieve the anxiety and worry that accompanies obsessions, or to prevent a feared outcome, such as illness. Compulsions are distressing and time consuming, and can interfere with day to day routines and living.
Washing & Cleaning
- Washing hands / body in a certain way
- Doing things to prevent contact with germs / contaminants
Checking
- That you did something in a certain way / did not make a mistake
- That you did not harm others / yourself
Mental Compulsions
- Reviewing events to prevent negative consequences / harm
- Praying to prevent harm
- Counting to end on a ‘good’ or ‘right’ number
Repeating
- Activities (in / out of doors a certain number of times)
- Sequences of body movements (e.g., touching, tapping or blinking)
- Words (e.g., rereading, rewriting, or avoiding certain words / combinations of letters)
- ‘Multiples’ (e.g., doing something ‘3 times’ because it is ‘safe’)
Others
- Hoarding, saving or collecting compulsions
- Avoiding situations that might trigger your obsessions
- Ordering or rearranging things until it ‘feels right’
- Confessing, to receive reassurance
Compulsive Behaviors Similar to OCD
Trichotillomania is a body-focused repetitive behavior characterized by recurrent, irresistible urges to pull out hair from the scalp, eyebrows, eyelashes, or other areas, leading to noticeable hair loss. While distinct from OCD, it shares features such as difficulty resisting urges and is often triggered by stress or negative emotions. Individuals may experience shame, low self-esteem, and social withdrawal.
Misophonia (‘hatred of sound’) is a condition related to compulsive-like behaviours but is not classified as OCD. It shares some features with anxiety disorders, such as avoidance, for many who experience it. People with misophonia have strong, distressing emotional reactions—like irritation or anger—to common sounds (e.g., chewing or breathing), often leading to urges to avoid or escape those situations. There is also evidence suggesting misophonia has a significant hereditary component.
Although both difficulties can involve anxiety and avoidance, they differ from OCD in their underlying patterns and how these urges manifest, requiring tailored approaches to support people and their treatment. Often people can benefit from practising specific self-regulation skills, like urge-surfing, grounding, and graded exposure therapy.
If your mind keeps getting stuck on certain rules, beliefs, images, or thoughts — or if you feel compelled to act in rigid, inflexible ways that interfere with living a meaningful life — know that help is available. Effective treatments exist for OCD and related compulsive behaviours, and you don’t have to face this alone.
Other Anxiety Disorders are explained below:
- Intense excessive worry about social situations (Social Anxiety Disorder)
- Persistent, excessive or unrealistic worries (Generalized Anxiety Disorder)
- Panic attacks (Panic Disorder)
- An intense, irrational fear of everyday objects, animals, or situations (Specific Phobia)
- Upsetting memories and agitation or numbness following a traumatic event that interferes with ability to function in life (Post Traumatic Stress Disorder)
Resources
- Read more about Anxiety here
- Learn about your Window of Tolerance
- What is Mindfulness?
- Calm yourself with this powerful breathing technique
- Learn about your Brain’s 3 Emotion Regulation Systems
- Understanding the Physiology of Self-Criticism
- Fears of Compassion
- For a list of all Self-Help articles that I have written, visit this page

How to Get the Most Out of Therapy
Are you new to therapy? Working with a psychologist is very different to visiting a doctor. Learn about what to expect and how you can get the most out your therapy experience, here.

The Science of Behaviour Change: Understand & BreakPatterns
Struggling with repetitive behaviors like avoidance, self-criticism, or anxiety? Learn how to break free by understanding the underlying patterns. Discover practical strategies to intervene effectively and build healthier habits, here.

Exposure Therapy: Overcoming Anxiety, Fear & Discomfort
Exposure Therapy is a well-established psychological treatment with decades of success that has helped countless people regain confidence and control over their lives. This step-by-step guide will walk you through the basics of Exposure Therapy including how to incorporate complimentary skills to enhance its effectiveness.

Can AI Chatbots Harm Your Mental Health? Exploring the Risks
While AI may seem like a convenient source of support, it has important limitations and carries risks—especially when it comes to emotional wellbeing. If you’re struggling or in distress, the safest and most effective step is to seek help from a trained professional who offers personalised care and genuine human connection.

Blue Light, Melatonin, & Cognitive Stimulation: Why Technology Disrupts Sleep
Overview: Quality sleep is essential for mental health and overall wellbeing, supporting emotional regulation, cognitive function, and the body’s physical recovery processes. This article explains how evening exposure to screens and cognitive stimulation can disrupt melatonin production and sleep quality, and provides practical strategies to improve sleep hygiene and wind down effectively. Blue Light, Melatonin, […]
Understanding Your Window of Tolerance
Your Window of Tolerance is the zone of arousal in which you are able to function most effectively. The size of your Window of Tolerance depends on how much you can tolerate mild fluctuations in mood, energy levels, and the challenges and demands of life, whilst remaining in the Optimal Zone. Lean to work with your Window of Tolerance, here.

How EMDR Therapy Can Help Relieve Trauma-Related Distress
EMDR Therapy is an evidence-based approach that helps reprocess past distressing memories and supports relief from intrusive thoughts, nightmares, and unhelpful self-beliefs. Developed over 30 years ago to treat trauma, it is now used whenever memories cause significant physical or psychological distress

How Our Early Attachment Experiences Affect Us: Relationships, Growth & Healing
Attachment-related emotional learning that occurs in the first 15 years of life can either serve as a protective factor against life’s challenges or can lead to difficulties in emotion regulation, relationships, & mental health vulnerabilities carried into adulthood. Discover how your attachment experiences have shaped you and how you can begin to heal from the wounds of your past.

Your Brain’s 3 Emotion Regulation Systems
The majority of mental health problems relate to an imbalance of 3 very important systems. From anxieties about the future, or shame and rumination about the past; to attacking one’s self for our failures with harsh self-criticism. There is no peace when being driven by Threat! Learn how to soothe your Threat system so that you can comfort, soothe & support yourself.
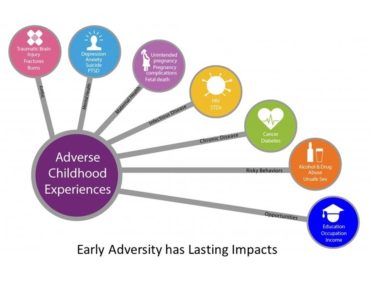
Adverse Childhood Experiences (ACEs)
Toxic stress from ACEs can change the brain, effectively narrowing our Window of Tolerance and making us susceptible to chronic mental health and medical conditions. Effects of toxic stress can be passed on intergenerationally, but can also be significantly lessened by protective factors. Learn about ACEs and what you can do to help yourself, here.

Your Brain’s Threat System
Your threat system is designed to protect you from danger. It is about SURVIVAL! However, excessive threat can overwhelm us and can spiral into hopelessness & self-criticism. Learn about how to manage your threat system here.

Negative Thinking – What your poor brain doesn’t know…
When we are on ‘autopilot’ we are often unaware that our mind’s focus can be threatening and that this is contributing to psychological distress. Conversely, the information from our 5 senses is generally an untapped haven of calm, soothing, stillness and peace – Learn how you can use this knowledge to your advantage to free yourself from overthinking.
Soothing Rhythm Breathing
Many clients report that this breathing technique is one of the most helpful emotion-regulation skills that they learn in therapy. Learn to quickly deactivate your ‘fight/flight’ response & activate your soothing system with this powerful breathing technique.

Choosing What Truly Matters, Even When It’s Hard
Are you stuck making the same choices over and over, even though this is not helping you move towards what you want in life? Learn practical ways to decide what is most important to you and how to keep yourself on track, here.

What is Mindfulness ?
Mindfulness can increase self-awareness, can help you self-regulate & can help you choose how best to respond to challenging situations. But Mindfulness is hugely misrepresented and many false claims abound. Although mindful awareness is essential, Mindfulness alone is not enough. Learn what Mindfulness is, how to make use of it, and what else you need in order to make positive changes, here…

Common Obstacles in Learning Mindfulness
People encounter common obstacles when trying to learn Mindfulness. You can save yourself time, effort & frustration by understanding and planning for these difficulties. Enjoy the maximal benefits of Mindfulness with least amount of effort, here.

Guided Mindfulness Audio Exercises
Access guided Mindfulness exercises here. Increase your awareness, improve your resilience. Learn how to respond (vs react). Cultivate inner-peace, now.

Mindfulness & Your DNA
People who engage in a regular mindfulness practice are more likely to process (than avoid) their emotions, and report less stress and increased happiness. The benefits of regular mindfulness practice can now be measured at the DNA level. Take a closer look here.

The Physiology of Self-Criticism
Self-criticism activates the threat system and is a common problem across all mental health difficulties. Learn about the powerful effects of self-criticism on your emotions, your brain, and your physiology. Also learn about your most powerful antidote: Self-compassion.

Understanding Your ‘Inner-Critic’
‘Self-talk’ is great when it helps us – but self-criticism can be painful and destructive! If you speak to yourself in judgmental, shaming, self-critical, or hurtful ways – this is likely the voice of your ‘inner-critic’. Learn helpful ways of responding to your ‘inner-critic’ here…

Compassion – A brief overview
Compassion is one of the most beneficial things from psychological science that you can learn – but unfortunately it is also poorly misunderstood. Compassion does NOT mean ‘being nice’ or ‘having empathy’ – This article will discuss what compassion is and how it can help you reduce your suffering.

The Benefits of Self-Compassion
Self-compassion is one of most helpful (but most difficult) of all psychological skills. Self-compassion can help you work with difficult feelings such as anger and intense shame or harsh self-criticism, and unlike your inner-critic, self-compassion can help you soothe and nurture yourself when you are at your most distressed. However, often due to our upbringing and due to commonly held myths around it – self-compassion is typically misunderstood, feared, avoided or blocked. Learn what self-compassion is, how it gets blocked, & how you can help yourself, here.

Fears, Blocks & Resistances to Compassion
Compassion requires awareness, immense courage and specific skills. However, often due to our emotional learning, many of us react with fears, blocks & resistances. Learn about why this is, and how you can allow more of this light in.

How to Get a Better Night’s Sleep
Having trouble sleeping? Poor sleep increases irritability, reduces concentration & can negatively affect our mood. Use the following tips to improve your sleep today!

Heart Rate Variability & Mental Health
Heart Rate Variability (HRV) is a measure of your ability to handle psychological stress. Low HRV is related to negative emotions such as anger, depression, anxiety, rumination, and self-criticism. Learn about HRV and how you can easily improve it and increase your ability to handle stress and difficult emotions, here.

The Mental Health Benefits of Nature
Nature is good for our mental and physical health. Exposure to Nature can have powerful restorative effects that promote recovery from physiological and psychological stress. Discover ways you can immerse yourself in nature, and cultivate a state of mind that is most receptive to its benefits.

How to Get the Most Out of Therapy
Are you new to therapy? Working with a psychologist is very different to visiting a doctor. Learn about what to expect and how you can get the most out your therapy experience, here.

Blue Light, Melatonin, & Cognitive Stimulation: Why Technology Disrupts Sleep
Overview: Quality sleep is essential for mental health and overall wellbeing, supporting emotional regulation, cognitive function, and the body’s physical recovery processes. This article explains how evening exposure to screens and cognitive stimulation can disrupt melatonin production and sleep quality, and provides practical strategies to improve sleep hygiene and wind down effectively. Blue Light, Melatonin, […]

Exposure Therapy: Overcoming Anxiety, Fear & Discomfort
Exposure Therapy is a well-established psychological treatment with decades of success that has helped countless people regain confidence and control over their lives. This step-by-step guide will walk you through the basics of Exposure Therapy including how to incorporate complimentary skills to enhance its effectiveness.

Can AI Chatbots Harm Your Mental Health? Exploring the Risks
While AI may seem like a convenient source of support, it has important limitations and carries risks—especially when it comes to emotional wellbeing. If you’re struggling or in distress, the safest and most effective step is to seek help from a trained professional who offers personalised care and genuine human connection.

The Science of Behaviour Change: Understand & BreakPatterns
Struggling with repetitive behaviors like avoidance, self-criticism, or anxiety? Learn how to break free by understanding the underlying patterns. Discover practical strategies to intervene effectively and build healthier habits, here.
Understanding Your Window of Tolerance
Your Window of Tolerance is the zone of arousal in which you are able to function most effectively. The size of your Window of Tolerance depends on how much you can tolerate mild fluctuations in mood, energy levels, and the challenges and demands of life, whilst remaining in the Optimal Zone. Lean to work with your Window of Tolerance, here.

How EMDR Therapy Can Help Relieve Trauma-Related Distress
EMDR Therapy is an evidence-based approach that helps reprocess past distressing memories and supports relief from intrusive thoughts, nightmares, and unhelpful self-beliefs. Developed over 30 years ago to treat trauma, it is now used whenever memories cause significant physical or psychological distress

How Our Early Attachment Experiences Affect Us: Relationships, Growth & Healing
Attachment-related emotional learning that occurs in the first 15 years of life can either serve as a protective factor against life’s challenges or can lead to difficulties in emotion regulation, relationships, & mental health vulnerabilities carried into adulthood. Discover how your attachment experiences have shaped you and how you can begin to heal from the wounds of your past.

Your Brain’s 3 Emotion Regulation Systems
The majority of mental health problems relate to an imbalance of 3 very important systems. From anxieties about the future, or shame and rumination about the past; to attacking one’s self for our failures with harsh self-criticism. There is no peace when being driven by Threat! Learn how to soothe your Threat system so that you can comfort, soothe & support yourself.

Adverse Childhood Experiences (ACEs)
Toxic stress from ACEs can change the brain, effectively narrowing our Window of Tolerance and making us susceptible to chronic mental health and medical conditions. Effects of toxic stress can be passed on intergenerationally, but can also be significantly lessened by protective factors. Learn about ACEs and what you can do to help yourself, here.

Your Brain’s Threat System
Your threat system is designed to protect you from danger. It is about SURVIVAL! However, excessive threat can overwhelm us and can spiral into hopelessness & self-criticism. Learn about how to manage your threat system here.

Negative Thinking – What your poor brain doesn’t know…
When we are on ‘autopilot’ we are often unaware that our mind’s focus can be threatening and that this is contributing to psychological distress. Conversely, the information from our 5 senses is generally an untapped haven of calm, soothing, stillness and peace – Learn how you can use this knowledge to your advantage to free yourself from overthinking.

Soothing Rhythm Breathing
Many clients report that this breathing technique is one of the most helpful emotion-regulation skills that they learn in therapy. Learn to quickly deactivate your ‘fight/flight’ response & activate your soothing system with this powerful breathing technique.

Choosing What Truly Matters, Even When It’s Hard
Are you stuck making the same choices over and over, even though this is not helping you move towards what you want in life? Learn practical ways to decide what is most important to you and how to keep yourself on track, here.

What is Mindfulness ?
Mindfulness can increase self-awareness, can help you self-regulate & can help you choose how best to respond to challenging situations. But Mindfulness is hugely misrepresented and many false claims abound. Although mindful awareness is essential, Mindfulness alone is not enough. Learn what Mindfulness is, how to make use of it, and what else you need in order to make positive changes, here…

Common Obstacles in Learning Mindfulness
People encounter common obstacles when trying to learn Mindfulness. You can save yourself time, effort & frustration by understanding and planning for these difficulties. Enjoy the maximal benefits of Mindfulness with least amount of effort, here.

Guided Mindfulness Audio Exercises
Access guided Mindfulness exercises here. Increase your awareness, improve your resilience. Learn how to respond (vs react). Cultivate inner-peace, now.

Mindfulness & Your DNA
People who engage in a regular mindfulness practice are more likely to process (than avoid) their emotions, and report less stress and increased happiness. The benefits of regular mindfulness practice can now be measured at the DNA level. Take a closer look here.

The Physiology of Self-Criticism
Self-criticism activates the threat system and is a common problem across all mental health difficulties. Learn about the powerful effects of self-criticism on your emotions, your brain, and your physiology. Also learn about your most powerful antidote: Self-compassion.

Understanding Your ‘Inner-Critic’
‘Self-talk’ is great when it helps us – but self-criticism can be painful and destructive! If you speak to yourself in judgmental, shaming, self-critical, or hurtful ways – this is likely the voice of your ‘inner-critic’. Learn helpful ways of responding to your ‘inner-critic’ here…

Compassion – A brief overview
Compassion is one of the most beneficial things from psychological science that you can learn – but unfortunately it is also poorly misunderstood. Compassion does NOT mean ‘being nice’ or ‘having empathy’ – This article will discuss what compassion is and how it can help you reduce your suffering.

The Benefits of Self-Compassion
Self-compassion is one of most helpful (but most difficult) of all psychological skills. Self-compassion can help you work with difficult feelings such as anger and intense shame or harsh self-criticism, and unlike your inner-critic, self-compassion can help you soothe and nurture yourself when you are at your most distressed. However, often due to our upbringing and due to commonly held myths around it – self-compassion is typically misunderstood, feared, avoided or blocked. Learn what self-compassion is, how it gets blocked, & how you can help yourself, here.

Fears, Blocks & Resistances to Compassion
Compassion requires awareness, immense courage and specific skills. However, often due to our emotional learning, many of us react with fears, blocks & resistances. Learn about why this is, and how you can allow more of this light in.

How to Get a Better Night’s Sleep
Having trouble sleeping? Poor sleep increases irritability, reduces concentration & can negatively affect our mood. Use the following tips to improve your sleep today!

Heart Rate Variability & Mental Health
Heart Rate Variability (HRV) is a measure of your ability to handle psychological stress. Low HRV is related to negative emotions such as anger, depression, anxiety, rumination, and self-criticism. Learn about HRV and how you can easily improve it and increase your ability to handle stress and difficult emotions, here.

The Mental Health Benefits of Nature
Nature is good for our mental and physical health. Exposure to Nature can have powerful restorative effects that promote recovery from physiological and psychological stress. Discover ways you can immerse yourself in nature, and cultivate a state of mind that is most receptive to its benefits.
Dr Andreas Comninos
PhD Clinical Psychologist
EMDRAA Accredited Practitioner | Psychology Board Approved Supervisor
Hello, I’m Dr. Andreas Comninos, a PhD Clinical Psychologist with over 15 years of experience supporting people through meaningful psychological change. My goal is to provide a safe, respectful space where we can work collaboratively—setting clear goals and exploring your experiences in depth.
Drawing on the latest evidence-based approaches, I integrate mind-body practices to help address complex emotions and unhelpful patterns.
My PhD research, completed at the University of Wollongong (2008), explored how attachment styles influence not just how quickly—but how fully—we recover in therapy. These insights continue to guide the way I work, across all therapeutic approaches and interventions. You can learn more about this research here.
In our sessions, I aim to help you feel seen, safe, and understood—core elements of secure attachment. We’ll tailor interventions to your needs and goals, and work together to strengthen your relationship with yourself and others—fostering resilience and lasting change.
Medicare rebates are available Australia-wide for up to 10 sessions per calendar year with a GP referral and Mental Health Care Plan. Rebates also apply for for Private Health, NDIS, and DVA Gold Card holders.
To book an appointment please reach out using the contact details below. You’re welcome to share your goals or what you’d like support with—I look forward to hearing from you.
If you’re not quite ready to start therapy, I invite you to explore the self-help articles I’ve written—they’re designed to offer practical support and insights you can use right away.

Dr Andreas Comninos
B.Psych (Hons), PhD (Clin Psych), MAPS
- PhD Clinical Psychologist
- EMDR Therapist | EMDRAA Accredited Practitioner
- Psychology Board Approved Supervisor

Dr Andreas Comninos
B.Psych (Hons), PhD (ClinPsych), MAPS
- PhD Clinical Psychologist
- EMDR Therapist | EMDRAA Accredited Practitioner
- Psychology Board Approved Supervisor
- 15+ years experience
About Andreas
Hello, I’m Dr. Andreas Comninos, a PhD Clinical Psychologist with over 15 years of experience supporting people through meaningful psychological change. My goal is to provide a safe, respectful space where we can work collaboratively—setting clear goals and exploring your experiences in depth.
Drawing on the latest evidence-based approaches, I integrate mind-body practices to help address complex emotions and unhelpful patterns.
My PhD research, completed at the University of Wollongong (2008), explored how attachment styles influence not just how quickly—but how fully—we recover in therapy. These insights continue to guide the way I work, across all therapeutic approaches and interventions. You can learn more about this research here.
In our sessions, I aim to help you feel seen, safe, and understood—core elements of secure attachment. We’ll tailor interventions to your needs and goals, and work together to strengthen your relationship with yourself and others—fostering resilience and lasting change.
Medicare rebates are available Australia-wide for up to 10 sessions per calendar year with a GP referral and Mental Health Care Plan. Rebates also apply for for Private Health, NDIS, and DVA Gold Card holders.
To book an appointment please reach out using the contact details below. You’re welcome to share your goals or what you’d like support with—I look forward to hearing from you.
If you’re not quite ready to start therapy, I invite you to explore the self-help articles I’ve written—they’re designed to offer practical support and insights you can use right away.
Appointment Enquiries
Online Psychology Services, Sydney & Australia-wide